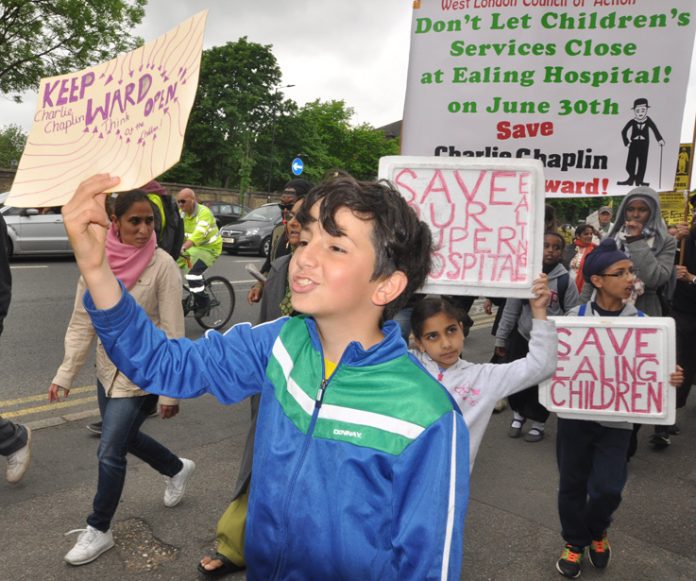THE low priority given to children and young people’s health threatens prosperity, argues an expert writing in The BMJ Today.
Professor Russell Viner at University College London’s Institute of Child Health, says countries that invest in child health ‘reap impressive economic rewards, with each pound spent on children’s health returning over £10 to society over a lifetime’. In contrast, poor health in childhood ‘leads to reduced workforce participation and productivity and lowers national wealth’.
Professor Viner, who takes up the role of president of the Royal College of Paediatrics and Child Health this week, points out that the UK has a higher proportion of children and young people in its population than almost all other Western European countries that will provide us ‘a future demographic dividend of a larger working-age population if, and only if, we protect their health’.
But he argues that ‘we are poorly positioned to reap these benefits, as our children’s health outcomes are substantially worse than those in most other wealthy European countries’. He points out that Scotland and Wales have both recently announced new national strategies to improve children’s health. Yet in England, health services for children and young people ‘struggle for priority and there is no sign yet of a national strategy’.
For example, the NHS Five Year Forward View mentions children and young people briefly only in relation to prevention and mental health, while the 2016 General Practice Forward View mentions children only once, despite children making up a large proportion of primary care attendances. And although patients aged 0-18 years made up 25% of A&E attendances in 2015-16, the 2013 Transforming Urgent and Emergency Care Services in England mentions this group briefly twice.
This lack of focus has begun to tell, writes Viner.
Across the UK, large gaps in the paediatric workforce have lowered morale in children’s services, recruitment into paediatric training positions. 2017 was the worst ever, and workforce deficiencies, low morale and lack of focus on children are cited as reasons for large numbers of services receiving poor ratings for safety and effectiveness.
He says the moral and economic reasons for action are clear, and he calls for ‘a new focus on health services for the children and young people who carry all our futures’. For each UK country this means a targeted health strategy, formulated in partnership with children and their families, and covering early life from from conception to adulthood.
For England it also means a greater visibility within NHS England priorities in primary care and emergency care and in the new integrated care systems. ‘The Royal College of Paediatrics & Child Health is keen to work with governments to achieve these aims. Business as usual for child health will not build a healthy and prosperous United Kingdom,’ he concludes.
Meanwhile, ‘socioeconomic inequalities in survival remain a major public health problem,’ the BMJ today has also found. The study finds little evidence for any direct impact of national cancer policy initiatives implemented since 2000 on short term cancer survival in England.
And no evidence was found for a reduction in social and economic inequalities (‘deprivation gap’) in cancer survival since the mid-1990s. The researchers say that these findings ‘emphasise that socioeconomic inequalities in survival remain a major public health problem for a healthcare system founded on equity’.
Cancer survival in England has been improving steadily since the 1970s, but still lags behind that seen in comparable countries in Europe. Differences in cancer survival between less and more deprived patients also persist for most types of cancer.
The NHS Cancer Plan was launched in 2000 in a bid to tackle these inequalities and improve cancer survival to levels comparable with the rest of Europe. Since then, other strategies have been introduced, but little is known about their impact at a national level. So researchers in the Cancer Survival Group at the London School of Hygiene & Tropical Medicine set out to assess the impact of the NHS Cancer Plan and subsequent strategies on cancer survival in England and whether any gains were evenly distributed across the socio-economic groups of the population.
They analysed national cancer registry data for 3.5 million people aged 15-99 who had been diagnosed with one of the 24 most common cancers in three pre-defined calendar periods: 1996-2000, 2001-05, and 2006-13 with follow-up to 2014. This allowed comparison of trends before and after introduction of the NHS Cancer Plan.
They then estimated one year net survival for each cancer by sex, year of diagnosis, and level of deprivation. They focused on one year survival because most inequalities in cancer survival in England arise shortly after diagnosis. They found that one year survival improved steadily from 1996 for 26 of 41 sex-cancer combinations studied.
For nine additional cancers, improvement in survival was initially negligible, and really began or accelerated only later, from 2001 or 2006. The largest improvements (greater than 1% per year) were seen for cancers that were of poor or intermediate prognosis in the 1990s, such as cancers of the oesophagus and liver in men, lung in women, and kidney, mesothelioma, and myeloma.
In contrast, survival for men diagnosed as having cancer of the larynx or testis, or Hodgkin lymphoma, was already high in the 1990s, and this improved little by 2013. Meanwhile, the deprivation gap remained unchanged for most cancers, with a clear, persistent pattern of lower survival among more deprived patients.
While the gap narrowed slightly for some cancers, where one year survival was already more than 65% in 1996, it widened notably for brain tumours in men and for lung cancer in women. The researchers point to some limitations and say their study may be too early to detect the full impact of recently implemented cancer initiatives.
Nevertheless, the study is based on virtually all cancer cases registered in England over 18 years, allowing for more accurate estimates of trends. ‘Even though increasing cancer survival and reducing inequalities in survival have been among the main targets of national cancer policy initiatives implemented since 2000, this study found little evidence of a direct impact of these strategies on one year survival, and no evidence for a reduction in socioeconomic inequalities in survival,’ write the authors.
They say their findings ‘should be taken into consideration by cancer policy makers and inform future initiatives’ and suggest that ‘shifting the focus from individual factors to healthcare system factors might prove to be beneficial in improving cancer outcomes among the most disadvantaged.’
Does this mean the NHS cancer reforms failed, ask researchers at the University of Otago, New Zealand, in a linked editorial? They point out that drivers of social disparities in cancer outcomes are complex, making it difficult to establish cause and effect, and they say genuine improvements ‘may require a more comprehensive approach than the NHS reforms’.
To reduce the incidence and impact of cancer ‘we must continue to be ambitious,’ they write. ‘The goals of the NHS Cancer Plan were to save lives and to ensure that the gains were evenly shared. These goals remain critical. The methods to achieve them need more work,’ they conclude.